USA Burnout Retreats & Therapy: Comparative Analysis
The Landscape of Occupational Burnout Interventions in the United States: A Comparative Analysis of Therapeutic Modalities and Intensive Retreats

Introduction to the Occupational Burnout Epidemic
Over the past decade, occupational burnout has evolved from a colloquial descriptor for general fatigue into a severely debilitating systemic condition with profound clinical, economic, and social implications across the United States. In 2019, the World Health Organization (WHO) formally recognized burnout in the International Classification of Diseases (ICD-11), defining it exclusively as an “occupational phenomenon” resulting from chronic workplace stress that has not been successfully managed. This vital reclassification shifted the clinical and cultural paradigm of burnout from a perceived personal failing or lack of individual resilience to a structural and systemic issue affecting massive segments of the American workforce. This phenomenon is particularly acute in high-stress environments such as healthcare, corporate executive leadership, and frontline services.
The systemic ramifications of this condition extend far beyond individual distress, creating cascading failures within critical national infrastructures. The American healthcare system, for instance, faces unprecedented challenges due to physician and nurse burnout. Contemporary studies indicate that approximately 63% of practicing physicians in the United States report experiencing burnout symptoms at least once a week. In specialized fields such as physical therapy, longitudinal research stretching back to the 1980s has consistently shown high levels of emotional exhaustion, with more recent data indicating that professionals in these roles suffer from severe depletion of personal coping resources. This epidemic among medical practitioners leads directly to an increase in medical errors, reduced patient satisfaction, staffing shortages, and massive turnover, severely compromising the quality of care delivery.
Similarly, within the corporate sector, executive burnout severely compromises strategic decision-making, emotional intelligence, and overall leadership efficacy. A recent survey highlighted that more than 80% of white-collar workers experience at least one mental health symptom linked to occupational stress, while roughly half of all executives experience significant, debilitating stress. High-achieving professionals often normalize these symptoms, remaining highly functional and successful “on paper” while internally operating in a state of chronic survival mode. These individuals are frequently plagued by emotional numbness, sleep disruption, and a complete inability to disconnect from their professional identities. As a result, the boundary between professional responsibility and self-neglect is entirely erased.
In response to this escalating crisis, the behavioral health sector in the United States has developed a highly bifurcated and specialized intervention landscape. On one end of the spectrum is sustained, community-based outpatient therapy, ranging from traditional weekly private practice sessions to virtual Intensive Outpatient Programs (IOP). On the other end are immersive, high-acuity interventions, including short-term wellness retreats focused on rapid nervous system regulation and extended residential rehabilitation programs tailored specifically for executives and licensed professionals. This report provides an exhaustive, evidence-based analysis of these modalities, comparing their clinical methodologies, neurobiological efficacy, economic structures, and long-term sustainability to offer a comprehensive understanding of burnout treatment in the modern American context.
The Neurobiological and Physiological Pathology of Burnout
To effectively evaluate the various treatment modalities for occupational burnout, it is first necessary to understand the clinical pathology and biological mechanisms of the condition. Burnout is not merely extreme tiredness; it is a complex systemic breakdown that impacts the individual across emotional, physical, mental, and spiritual dimensions, fundamentally altering the body’s physiological baseline.
When individuals endure ongoing occupational stress or corporate burnout, their body’s stress response system—specifically the hypothalamic-pituitary-adrenal (HPA) axis—remains in a state of constant activation. This prolonged exposure to stress hormones, primarily cortisol and adrenaline, leads to a sustained inflammatory response throughout the body. Over time, this chronic activation overwhelms the brain’s neurobiological capacity to manage stress, depleting critical neurotransmitters such as serotonin and dopamine, which are foundational for mood regulation, executive function, and motivation.
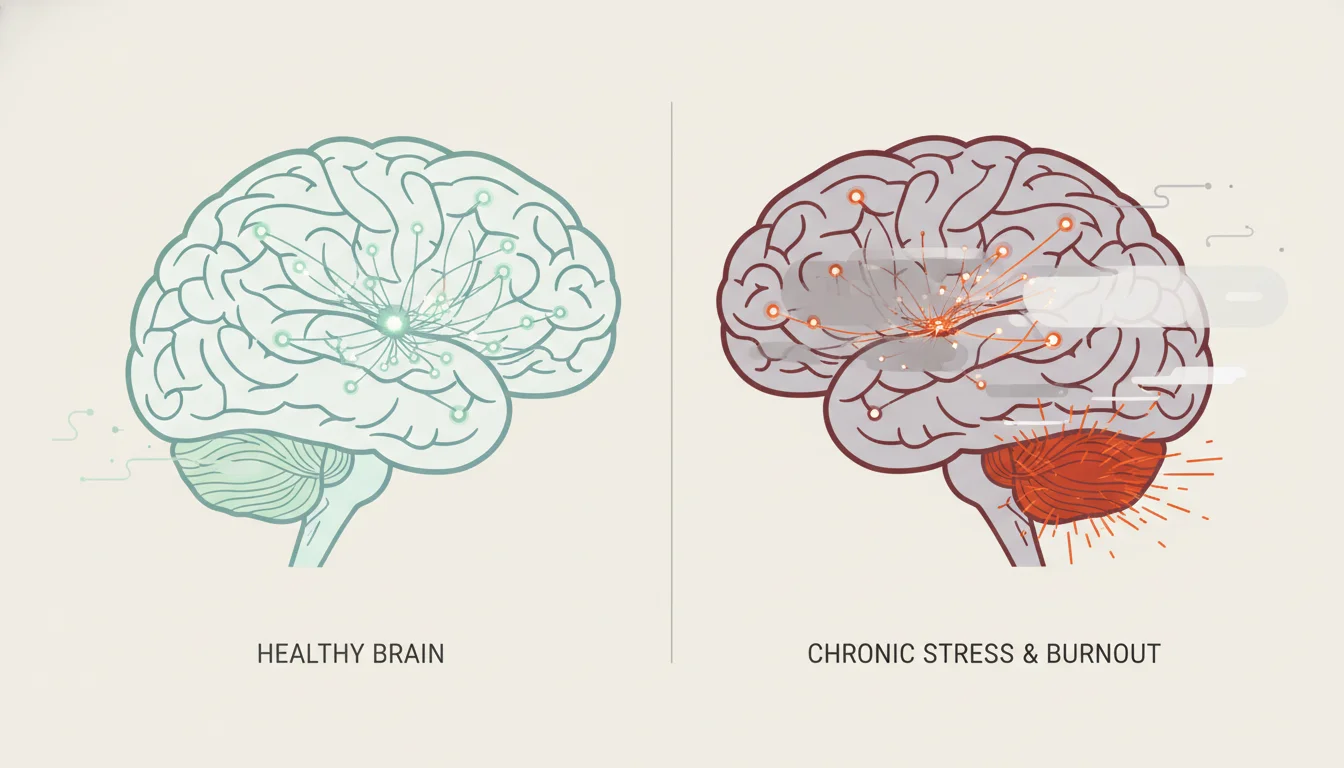
Consequently, the pathophysiology of burnout fundamentally rewires the brain’s architecture. Prolonged occupational stress has been shown to reduce gray matter density in the prefrontal cortex, the area of the brain responsible for complex cognitive behavior, decision-making, and moderating social behavior. Simultaneously, chronic stress enlarges and hyper-sensitizes the amygdala, the region that processes fear and threat. This architectural shift explains why individuals with severe burnout cannot simply “rest” or “sleep” their way to recovery; their baseline neurological state has been altered to perceive constant threat, rendering traditional relaxation techniques entirely ineffective and leading to a restless inability to find calm.
The clinical presentation of this neurobiological shift clusters into several multidimensional symptom categories. Mentally and emotionally, individuals exhibit a triad of core dimensions: severe emotional exhaustion, depersonalization (a growing cynicism and detachment toward one’s job and colleagues), and a markedly reduced sense of personal accomplishment. This emotional depletion drastically alters how professionals interact with their spouses, children, and peers, often leading to deep isolation, profound irritability, and a loss of motivation.
Physically, the somatic manifestations of burnout are profound and potentially life-threatening. The chronic sympathetic nervous system engagement (the “fight or flight” response) causes continuous physical strain, resulting in tension headaches, gastrointestinal distress, heart palpitations, chronic muscle pain, dizziness, nausea, and significantly compromised immune function. Spiritually and existentially, the condition erodes personal identity and values. Work begins to crowd out joy and health, leaving the individual feeling trapped, stuck, or behind despite outward success, ultimately cementing the belief that their entire self-worth is dictated solely by their corporate output.
Furthermore, burnout frequently acts as a precursor to, or catalyst for, severe clinical psychiatric disorders. The exhaustion and depletion of neurotransmitters drastically increase vulnerability to Major Depressive Disorder, Generalized Anxiety Disorder (GAD), and severe panic disorders. The inability to naturally self-regulate the nervous system often drives individuals toward maladaptive coping mechanisms. What begins as an attempt to self-medicate the anxiety and insomnia with alcohol or prescription drugs can rapidly evolve into chemical dependence, establishing a direct clinical pipeline between corporate burnout and severe substance use disorders (SUD).
Sustained Outpatient Therapy: Clinical Methodologies and Boutique Practices
Core Therapeutic Modalities for Burnout
Clinical practitioners deploy a variety of highly targeted interventions to address the specific cognitive and somatic presentations of burnout. Cognitive Behavioral Therapy (CBT) serves as a foundational approach in treating the cognitive distortions associated with chronic stress. CBT focuses on the interconnection between thoughts and behaviors, aiming to identify internal negative thought patterns—such as perfectionism, impostor syndrome, or the belief that one must always be productive—and challenging their validity. By practicing cognitive restructuring and exposure techniques, patients learn to replace destructive, self-critical thoughts with active problem-solving skills, ultimately shifting the brain away from a state of constant, perceived failure.
Dialectical Behavior Therapy (DBT), originally developed for borderline personality disorder, has proven highly efficacious for burnout recovery due to its intense focus on emotional regulation and distress tolerance. In the context of occupational stress, DBT equips professionals with critical interpersonal effectiveness skills, teaching them how to assert their needs, establish firm boundaries, and say “no” respectfully without internalizing guilt or causing professional harm. It heavily emphasizes mindfulness, training the patient to accept their current reality without judgment while working toward behavioral change.
For professionals whose burnout is intertwined with toxic workplace environments or occupational trauma, Eye Movement Desensitization and Reprocessing (EMDR) is increasingly utilized. Chronic stress can mimic the neurobiological effects of acute trauma.
EMDR utilizes bilateral stimulation across an eight-phase protocol to help professionals safely reprocess lingering pain, dysfunction, and negative self-beliefs acquired during their careers, replacing them with adaptive, positive core beliefs.
Acceptance and Commitment Therapy (ACT) is heavily utilized to help clients clarify their core values and reduce self-judgment. Instead of fighting anxiety, ACT encourages psychological flexibility, helping burned-out professionals reconnect with values beyond mere productivity and make meaningful behavioral shifts aligned with their authentic selves. Finally, recognizing that burnout is stored in the physical body, Somatic Experiencing and other body-based therapies focus directly on the nervous system. These therapies address how stress affects physiological sensations, guiding the body back to its ability to self-regulate and safely discharging the pent-up fight-or-flight energy that causes physical exhaustion.
Boutique Private Practices and the High-Achieving Professional
The outpatient therapy landscape in the United States is heavily stratified by socioeconomic factors. In high-income metropolitan areas such as New York City, San Francisco, Chicago, Atlanta, and Austin, a sub-sector of “boutique” private practices has emerged to cater specifically to ambitious professionals, C-suite executives, and creatives.
Clinics such as Insight Therapy NYC specialize in treating individuals who are highly successful but internally depleted. Under the direction of licensed clinical psychologists like Dr. Logan Jones, these practices utilize accountability-focused, insight-driven approaches rather than mere stress-management platitudes. The clinical goal is not to force dramatic career resignations overnight, but to facilitate small, intentional behavioral shifts that compound over time, allowing the individual to tolerate uncertainty without overworking and to navigate the nonstop pace of city life.
Similarly, the Lincoln Park Therapy Group in Chicago provides evidence-based, relational therapy tailored to the unique experiences of high-performing adults. Founded by Nicolle Osequeda, LMFT, the practice integrates Dr. Brené Brown’s “Daring Way” methodology into burnout recovery. This highly experiential approach focuses on building shame resilience, exploring vulnerabilities, and identifying the specific thoughts and behaviors that drive toxic hustle. Furthermore, because occupational burnout frequently degrades marital and family systems, boutique practices often deploy specialized relational frameworks, such as Emotionally Focused Therapy (EFT) and the Gottman Method, to help partners move from burnout-induced distress and emotional disconnection back toward empathy and love.
A significant trend within these affluent markets is the surge in private-pay (out-of-pocket) therapy. High-achieving professionals increasingly view private-pay therapy as a strategic investment in sustainable performance and professional risk management. By entirely bypassing health insurance, these executives ensure absolute confidentiality. This prevents the creation of permanent diagnostic paper trails—such as an official diagnosis of Major Depressive Disorder or Generalized Anxiety Disorder—that could potentially surface during corporate board evaluations, corporate acquisitions, or partnership reviews.
Intensive Outpatient Programs (IOP) and Partial Hospitalization Programs (PHP)
Program Structure and Multidisciplinary Delivery
Intensive Outpatient Programs generally require patients to participate in therapeutic programming for three to four hours a day, three to five days a week, with the total program typically lasting between six and twelve weeks depending on clinical need. Partial Hospitalization Programs offer a step up in intensity, providing full-day programming (often five to six hours daily) while still allowing the patient to return to a private residence or a designated supportive sober living facility at night.
These programs are inherently multidisciplinary, offering a highly structured schedule that moves far beyond isolated talk therapy. The core components of a burnout-focused IOP include deep-dive individual psychotherapy sessions with primary clinicians, alongside psychiatric evaluations and continuous medical oversight to ensure that underlying clinical depression or anxiety is biologically managed.
Crucially, group therapy forms the backbone of the IOP experience. Facilitated by licensed therapists, group sessions provide healthy mirroring, allowing high-achieving professionals to recognize that their specific struggles with toxic productivity and exhaustion are shared by peers. This dynamic dramatically reduces the isolation and stigma of mental health disorders, fosters a sustainable community, and provides a structured platform to practice interpersonal effectiveness and receive constructive feedback. Additionally, programs incorporate heavy psychoeducation and skill-building workshops designed to equip participants with practical tools for setting boundaries, self-compassion, and replacing maladaptive coping mechanisms.
Specialized IOPs also cater to specific professions. BoardPrep Recovery Center in Florida, for instance, operates a Health Professional Program (PHP and IOP) specifically tailored for licensed healthcare providers. This program acknowledges the unique challenges faced by medical personnel, utilizing biomarker sampling and accountability tools to ensure safety, while focusing heavily on creating best-practice professional documentation that allows doctors and nurses to safely return to duty without regulatory penalties.
The Proliferation of the Virtual IOP (Tele-IOP)
The post-pandemic landscape has witnessed a massive proliferation of Virtual IOPs, which clinical studies and patient retention rates suggest are as effective as traditional in-person programs. Clinics such as Clear Behavioral Health in California operate comprehensive Tele-IOPs that allow frontline workers, caregivers, and corporate employees to receive high-acuity care via secure, HIPAA-compliant video conferencing platforms.
Virtual programs specifically address the logistical and psychological barriers inherent to burnout treatment. Burned-out individuals often lack the physical energy to commute to a clinical facility, and the virtual model completely eliminates this friction, alongside avoiding the triggers of public transit or waiting rooms. Furthermore, virtual IOPs offer highly flexible scheduling, including specific morning, afternoon, and evening tracks, enabling professionals to integrate intensive mental health treatment seamlessly alongside their ongoing occupational and caregiving responsibilities. These virtual programs provide the same multimodal approaches—including CBT, DBT, and somatic therapy—delivered by Master’s-level clinicians directly to the patient’s home.
The Paradigm of Burnout Retreats: Immersion and Neurological Reset

Contrasting sharply with the sustained, gradual, and highly cognitive approach of outpatient therapy is the burnout retreat—an intensive, immersive experience designed to remove the individual entirely from their stressful environment and force a rapid neurological and physiological reset. Retreats vary widely in scope, ranging from short three-day weekend interventions to extensive week-long holistic immersions, located in serene natural environments such as the Colorado Rockies, Sedona, Joshua Tree, and the coastal regions of Florida and international destinations.
The Mechanisms of Retreat Efficacy
The clinical philosophy underpinning burnout retreats relies on the concept of profound environmental interruption. By physically removing a person from their daily occupational triggers, the central nervous system is granted an unparalleled opportunity to down-regulate. The efficacy of these retreats is driven by several synergistic mechanisms:
Firstly, extensive clinical research indicates that pure nature immersion rapidly triggers the parasympathetic nervous system, leading to measurable drops in circulating cortisol levels, blood pressure, and resting heart rate. Secondly, many retreats enforce strict “off-grid” policies or digital detoxification. This forced disconnection from email, corporate messaging, and the constant barrage of digital demands directly addresses “tech-fatigue”. By eliminating screen-induced sympathetic arousal, the brain can reset its circadian rhythms, profoundly improving sleep architecture and reducing the inflammatory markers associated with chronic insomnia.
Thirdly, retreats rarely rely on traditional talk therapy alone. Instead, they combine mindfulness meditation, yoga, somatic movement, specialized breathwork, and clean, anti-inflammatory nutrition. This combination of physical and psychological interventions creates a synergistic therapeutic effect that far exceeds the benefits of single clinical interventions. High-end wellness resorts, such as Canyon Ranch, offer programs like the “Mindful Journey Retreat” and “Spa Renewal Retreat”, providing all-inclusive, expert-guided mindfulness practices, sleep hypnosis, and deeply restorative whole-body care in a non-group setting for executives needing to become “unstuck”.
Additionally, a growing sub-sector of the retreat market incorporates altered states and psychedelic-assisted therapies.
Retreats offering Psilocybin in Colorado or Ayahuasca in international settings (such as Portugal, Spain, and Costa Rica) aim to induce profound spiritual awakening experiences. Clinical studies indicate that these guided experiences can rapidly increase neuroplasticity and gray matter density in emotional regulation centers, effectively bypassing months or even years of cognitive resistance and providing massive breakthroughs in trauma and burnout processing.
Efficacy Comparison: Intensive Retreats vs. Sustained Therapy
The primary advantage of a structured mental health retreat is the rapid velocity of symptom relief. A single day at a highly structured clinical retreat can be the equivalent of two months of traditional weekly therapy sessions. This accelerated healing occurs because the therapeutic container is continuous; there is no time wasted “catching up” on the week’s events, and the patient does not have the opportunity to transition back into rigid defense mechanisms before the session ends. The patient remains in an open, highly neuroplastic state for consecutive days.
Clinical studies demonstrate that even a brief three-to-five-day retreat can significantly reduce emotional exhaustion and depersonalization, with notable improvements in inflammatory markers and metabolic health. In studies evaluating medical professionals participating in mindfulness retreats, improvements were not only noted in personal burnout metrics but also translated directly into stronger therapeutic relationships and greater presence with their own patients.
However, intensive retreat models possess inherent limitations regarding long-term sustainability. Research into therapeutic intensity tradeoffs reveals that while psychological benefits peak immediately post-retreat, they typically exhibit a gradual regression curve over the subsequent six to eight weeks. Without the active implementation of learned techniques and structured aftercare, the individual is highly susceptible to returning to their previous baseline upon re-entering the toxic workplace environment that originally caused the burnout. Therefore, behavioral health experts agree that while retreats are unparalleled for breaking severe acute momentum and resetting the nervous system, they must be paired with sustained, twice-weekly or weekly outpatient therapy to optimize long-term behavioral integration and prevent relapse.
Residential Executive Burnout Programs: High-Acuity Intervention
For executives, physicians, entrepreneurs, and high-level professionals whose burnout has metastasized into severe mental health crises, debilitating substance use disorders, or catastrophic life dysfunction, neither weekly therapy nor a brief wellness retreat is sufficient. This demographic requires specialized, long-term Residential Executive Burnout Programs.
These comprehensive programs provide 30-to-90-day inpatient immersions within highly discreet, luxury environments designed to cater specifically to the demands and sensibilities of high-achieving populations. Premier facilities include Bridges to Recovery in Los Angeles, BoardPrep Recovery Center in Tampa, Living at Reflections in Northern California, Dana Shores Recovery Center, and The Sanctuary at Sedona.
Clinical Structure and Advanced Modalities
Executive residential rehabs operate on a sophisticated medical model combined with deep holistic care. Upon admission, patients undergo comprehensive medical evaluations, neuropsychological testing, and psychiatric assessments to pinpoint the exact physiological and psychological dysfunctions. Because severe burnout is rarely isolated, these centers specialize in Dual Diagnosis—treating the occupational stress and emotional exhaustion simultaneously with co-occurring disorders such as alcohol dependence, cocaine addiction, severe PTSD, or bipolar disorder.
Treatment at these facilities is exceptionally intensive, often featuring a very low client-to-staff ratio (e.g., a maximum of six clients per residence at Bridges to Recovery) to ensure deep therapeutic work and highly personalized support. Patients may receive upwards of five individual psychotherapy sessions per week, combined with group support meetings, EMDR, and CBT.
Crucially, these top-tier programs deploy advanced medical technologies and neuromodulation to repair the damaged brain. BoardPrep Recovery Center, for instance, utilizes Transcranial Magnetic Stimulation (TMS), an FDA-approved therapy that uses magnetic fields to stimulate brain cells. TMS is used to target mood-regulating circuitry for treatment-resistant depression, and innovatively applied off-label to target the ventromedial prefrontal cortex to reduce drug cue reactivity and cravings in executives battling addiction. Similarly, The Sanctuary at Sedona integrates cutting-edge options like ketamine-assisted treatment and NAD+ intravenous drips, which support cellular brain repair, immunity boosting, and deep nervous system regulation.
Accommodating the High-Level Professional
A defining characteristic of executive residential programs is their deep understanding of the professional’s reality. Historically, executives avoided residential care for fear of losing their jobs, damaging their reputations, or abandoning their companies during critical junctures. Modern executive programs mitigate these structural barriers in several innovative ways:
Unlike traditional rehabilitation centers that strictly confiscate all electronics and cut patients off from the outside world, executive programs explicitly integrate the patient’s professional life into the recovery process. Facilities like Dana Shores and various programs in Colorado provide private workspaces, secure communication channels, and designated “technology hours” to allow CEOs and partners to fulfill critical professional obligations, send emails, and maintain their careers alongside their recovery.
Furthermore, these centers offer extreme discretion and confidentiality. Accommodations are highly secluded—often luxury estates in places like Marin County, Beverly Hills, or San Juan Capistrano—featuring spa-style baths, lush gardens, private chefs, and equine therapy. This ensures absolute anonymity, allowing professionals to seek help without fear of reputational damage. For licensed professionals (such as physicians or pilots) whose licenses are in jeopardy, programs provide forensic-style Independent Medical Evaluations (IMEs) and professional clinician-to-clinician handoffs, tailoring treatment with best-practice elements that result in defensible documentation allowing a safe return to duty.
The Holistic Ecosystem and Biohacking
To heal the profound physical devastation of prolonged corporate burnout, these facilities incorporate advanced holistic wellness ecosystems. The Sanctuary at Sedona, for example, operates a “Brain Body Recovery Lab” that utilizes biological data and “biohacking” to enhance cognitive function. This involves organic nutritional therapy designed to replenish magnesium, protein, and healthy fats to stabilize mood and energy levels. Physical therapies ranging from acupuncture and yoga to massage, sound baths, and infrared saunas ensure that the executive returns to the boardroom not merely sober or stable, but biologically optimized and deeply rested.
Professional Credentials in Burnout Therapy
| Credential | Professional Title | Educational Pathway | Therapeutic Focus and Scope regarding Burnout |
|---|---|---|---|
| MD / DO | Psychiatrist | 4 years Medical School + 4-year Psychiatric Residency | Holds the highest level of medical authority. Capable of diagnosing complex medical co-morbidities associated with burnout. Focuses on psychopharmacology, medication management, and oversees medical detox or advanced neuromodulation (TMS, Ketamine). |
| PhD / PsyD | Clinical Psychologist | Doctoral Degree (5-7 years) + 2,000-4,000 hours Supervised Clinicals | Conducts deep neuropsychological testing and diagnostic assessments. Often provides highly specialized, evidence-based psychotherapies for severe, complex burnout, personality disorders, and trauma. |
| LCSW | Licensed Clinical Social Worker | Master of Social Work (MSW) + 2-3 years clinical supervision | Views burnout through a comprehensive systemic lens, evaluating how workplace policies, family dynamics, diversity issues, and societal pressures contribute to the individual’s psychological distress. |
| LPC / LMHC | Licensed Professional Counselor / Mental Health Counselor | Master of Arts in Counseling + Supervised Clinicals | Provides direct clinical interventions (CBT, DBT). Highly focused on the helping relationship, building practical coping skills, and addressing the day-to-day behavioral symptoms of anxiety and occupational stress. |
| LMFT | Licensed Marriage and Family Therapist | Master’s in Marriage and Family Therapy + Supervised Clinicals | Specifically focuses on how occupational burnout is degrading the client’s marriage and family systems. Utilizes relational frameworks to repair trust, communication, and emotional damage caused by career stress. |
The most effective intensive programs and high-end boutique private practices utilize a multidisciplinary approach, ensuring that a patient has access to a comprehensive care team.
Economic Dimensions, Insurance Constraints, and the Cost of Care
The Escalating Cost of Outpatient Therapy
In the 2024–2025 landscape, the national average cost for a standard 45-to-60-minute therapy session ranged broadly from $100 to $250. Comprehensive data analyzing over 105 million therapy sessions revealed a consistent upward pricing pattern, with therapy rates climbing approximately 4% annually since 2019. This outpaced general inflation during several years, pushing the average blended cost of therapy (incorporating both private pay and insurance) to roughly $139 per session by 2024, representing a 13% increase over five years.
However, this national average severely obscures the economic reality in high-income metropolitan areas where burnout is most concentrated. In cities like New York, San Francisco, Silicon Valley, and Los Angeles, specialized burnout therapists operating private-pay models routinely charge between $150 and $288+ per session.
This mass migration of specialized therapists toward private-pay (out-of-network) models is structurally driven by declining and stagnant insurance reimbursement rates. In 2025, Medicare reduced reimbursement rates for mental health services by approximately 14%, and payments for specific time-based psychotherapy codes were cut by 3.4%. Private insurers have largely mirrored these Medicare cuts. With the average insurance reimbursement rate hovering around $119 per session compared to an average private-pay rate of $159, clinicians find that the math of running an insurance-based practice no longer adds up. Consequently, many highly qualified therapists are forced to abandon insurance networks to sustain their practices, inadvertently transforming high-quality, specialized burnout care into a luxury commodity accessible primarily to affluent professionals.
The Economics of Intensive Retreats and Residential Care
-
Short-Term Wellness Retreats
$1,000 – $3,000 (US) / €340 – €2,450 (EU)
3 to 6-day programs focusing on yoga, meditation, nature immersion, and basic digital detox. International variations may include neuroscience therapies or plant medicine.
-
Standard Residential Rehab (30 Days)
$5,000 – $20,000
Mid-tier residential care for burnout and co-occurring substance use. Heavily reliant on insurance coverage. Without insurance, inpatient care in states like Connecticut averages over $629 per day.
-
Executive/Luxury Residential (30 Days)
$30,000 – $80,000+
Premium facilities (e.g., The Sanctuary, Bridges to Recovery). Includes world-class psychiatric care, low client ratios, private suites, chef-prepared meals, TMS, IV therapy, and professional integration capabilities.
At the highest end of the spectrum, programs like The Retreat by Sheppard Pratt—a premier self-pay residential psychiatric program—charge $68,000 for an all-inclusive 20-day minimum stay, equating to a daily rate of $3,400. This fee covers 24/7 nursing care, comprehensive diagnostics, 35 hours a week of interdisciplinary programming, and extensive holistic therapies.
The Corporate Business Case for Burnout Intervention
While the upfront, out-of-pocket costs of treating burnout—particularly at the executive residential level—appear exorbitant to the individual, they are vastly eclipsed by the macroeconomic cost of untreated burnout to the corporate entity. Extensive human resources research indicates that the cost of turnover for a single highly trained professional, such as a specialized nurse, physician, or corporate executive, ranges from $46,100 to $88,000.
When accounting for the staggering loss of institutional knowledge, the direct financial cost of medical or strategic errors, and the organizational “trickle-down” effect—where a burned-out leader’s toxicity and erratic decision-making spread to and destabilize their entire reporting staff—the return on investment (ROI) for intervention becomes highly favorable. Funding a $20,000 residential program or a $5,000 intensive virtual IOP for a critical executive is a minor expense compared to the cost of replacing that individual. Consequently, progressive health systems and forward-thinking corporations are increasingly exploring systemic ways to subsidize, mandate, or directly fund comprehensive burnout recovery programs to protect their most vital human capital.
Strategic Synthesis and Conclusions
Occupational burnout is a profound neurophysiological and psychological condition that cannot be cured through simple time off, vacations, or superficial self-care platitudes. It represents a fundamental dysregulation of the central nervous system, a structural alteration of brain architecture, and the complete erosion of emotional resilience caused by chronic, unmanaged environmental stressors.
The comprehensive analysis of the current treatment landscape in the United States reveals that clinical efficacy depends entirely on accurately matching the intervention modality to the specific acuity and severity of the individual’s burnout.
For early-to-moderate burnout, sustained outpatient therapy, particularly leveraging cognitive restructuring (CBT), psychological flexibility (ACT), and somatic techniques, offers the best long-term prognosis. It allows individuals to systematically rewire their relationship with work, implement robust boundaries, and process stress in real-time. The rapid proliferation of virtual therapy and Tele-IOPs has democratized access to higher-acuity care for busy professionals, though declining insurance reimbursements threaten to isolate the most qualified providers within an exclusive private-pay ecosystem.
For acute, overwhelming exhaustion, immersive wellness and mental health retreats serve as unparalleled biological circuit-breakers. By combining profound nature immersion, strict digital detoxification, and intensive mindfulness, retreats can achieve weeks’ worth of neurological regulation in a matter of days. However, their efficacy is inherently fragile; without structured therapeutic integration and skills implementation upon returning home, the neurobiological gains inevitably regress.
For severe, co-morbid burnout—the executive crisis wherein occupational stress leads to severe depression, anxiety, or substance dependence—luxury residential programs provide indispensable, life-saving interventions. By integrating cutting-edge medical technologies, deep psychiatric oversight, and holistic rehabilitation in a highly confidential, career-accommodating environment, these programs salvage the lives and careers of the nation’s most highly stressed professionals.
Ultimately, the most sophisticated and clinically sound approach to occupational burnout is a hybrid model. The optimal recovery trajectory utilizes the profound, rapid physiological reset of an immersive retreat to break the crisis momentum, immediately followed by seamless integration into a sustained, specialized outpatient therapy program. As the modern American workplace continues to exert unprecedented demands on human cognition and endurance, the integration of these therapeutic modalities will remain a critical necessity for maintaining both individual health and broader macroeconomic stability.


